
After decades of studying and practicing medicine, Dr. Shenary Cotter hit a crisis point around 2017. She was burned out and ready to quit.
“I was done,” Cotter said. “I was just miserable.”
Despite the obstacles she’d had up to that point in her career, she’d persevered. Cotter felt that being a doctor was God’s plan for her life, but she still felt ready to stop practicing medicine.
Then she found the direct primary care model of medicine.
“It saved my career,” Cotter said.
Direct primary care (DPC) cuts insurance out of the picture, and the model has gained traction nationwide over the last decade. These practices number more than 1,500 in the continental U.S. and Washington, D.C., according to Direct Primary Care Frontier, an industry advocacy group.
Lawmakers have passed state and federal legislation that facilitates the growth of these practices. In 2018, the Florida Legislature clarified that DPC is not insurance or subject to the tax codes surrounding insurance. Other states have passed similar legislation, and Congress may soon follow suit at the federal level.
Cotter said the DPC model allows physicians to fill the role they signed up for in the first place—namely develop relationships with patients and help them live healthier lives. But she says the current insurance dominated system doesn’t allow for that.
In 2018 she teamed up with Dr. Althea Tyndall-Smith to start Gainesville Direct Primary Care Physicians. The doctors began accepting patients and growing, while taking care not to overload themselves. With time, the duo saw they could take on more patients.
“We find what our limit is,” Tyndall-Smith said. “Once we reach our limit, if that’s our limit and we can’t see people, then that’s what’s going to happen.”

Once the practice hit a certain number of patients, the two women added a third doctor.
“But we will never take on more patients than we can manage, and that’s one thing that we’ve promised,” Tyndall-Smith said.
The practice has grown to around 870 patients, a number they say leaves them plenty of flex room. If a patient calls or texts with an unexpected need, Tyndall-Smith said she typically sees them the same day, but always within two.
A typical insurance-based doctor’s office usually lacks that flexibility. If something unexpected happens, appointments are often already booked and patients wait, go to urgent care, or go untreated.
“The employers want us to see as many patients as we can and fill as many charges as we can to make them as much money as we can,” Cotter said, adding that it hurts the patient and turns the doctor into a factory worker. “That is a miserable existence.”
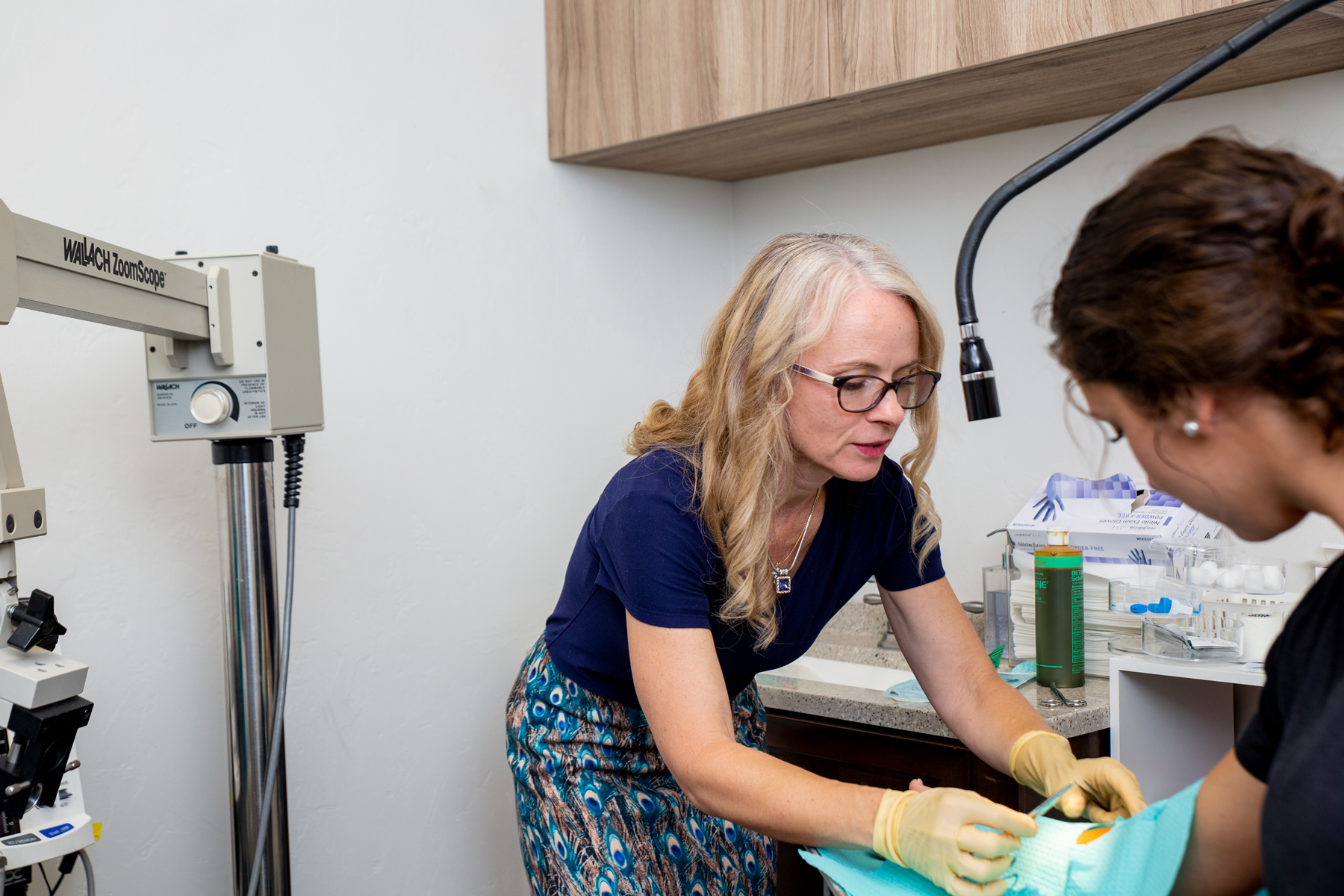
With DPC, doctors see fewer patients a day and can spend more time with each one. Cotter observed that after the 40-minute mark in a visit, patients often reveal crucial information about how they feel, which often ends up changing how she treats them.
She says patients need time to get comfortable with a doctor―time the current insurance model tries to reduce in order to see more patients.
In place of insurance, DPC comes at a flat monthly or yearly fee, for which patients have unlimited access to their doctor. At Gainesville DPC Physicians, a single adult pays $80 a month. Patients can schedule visits anytime without additional fees, and fewer patients makes unplanned visits easier to schedule.
Additional costs come if the patient needs a product or procedure from a third party, like medication or lab work. Cotter says those come at a reduced price because of the contracts the DPC clinic has secured.
As an example Cotter cited a patient who needed 40mg twice a day of omeprazole, a drug to treat stomach and esophagus problems. The over-the-counter cost is around $100 a month. Through Cotter, the patient got a six-month supply for $13.80.

DPC is still a fuzzy concept in the minds of many and not in widespread use compared to the insurance model. A 2018 poll from the Medical Group Management Association found that 74 percent of people were not aware of the DPC model.
Critics say the model increases disparities in health care and will cause a shortage of physicians, because DPC practices retain fewer patients than traditional practices. And while DPC doesn’t claim to be insurance, some argue it is simply unregulated insurance.
Cotter says the biggest obstacle to the model is the mental barrier most people have about it. Health insurance is so ingrained in people as a necessity that they can’t imagine going without it. But, she says, people don’t need health insurance—they just need health care.
Cotter said the clinic can cover 90 to 95 percent of their patients’ health care. They get the rest covered through either a catastrophic insurance policy or by joining a healthcare sharing ministry, which is what Cotter does for herself and her family.
“The vast majority of people, if they change their policy and get rid of their primary care coverage, they could pay for a membership with our practice in the money they save just from doing that,” Cotter said.

Suggested Articles
No related articles found.



