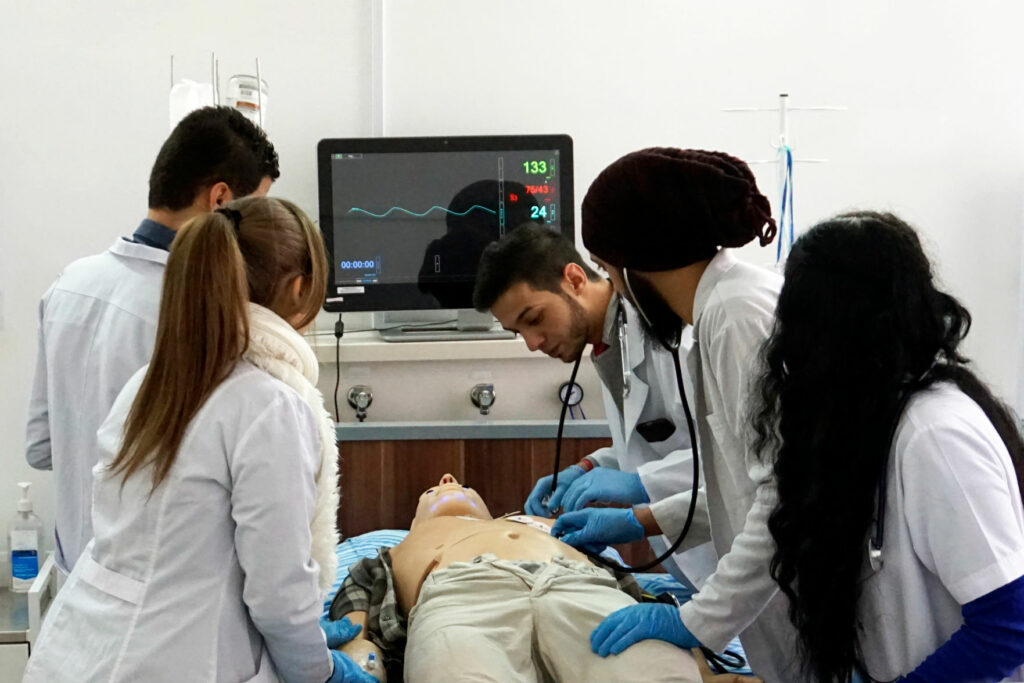
When a patient is in severe respiratory distress and needs to be put on a ventilator, health care providers race to insert a tube into their airway. But with COVID-19, a whole new checklist of critical, protective steps is needed at the start of that race to minimize the risk of spreading the virus.
At UF Health Shands, experts in interactive medical simulation are conducting realistic drills in the adult and pediatric emergency rooms and intensive care units to prepare for severe cases of the novel coronavirus./sites/default/files/media/TelehealthDemoPhoto2.jpg
Health care simulation, much like flight simulation, provides the opportunity to rehearse essential skills under realistic conditions, said Mary Patterson, M.D., M.Ed., associate dean of experiential learning in the UF College of Medicine, part of UF Health, and the Lou Oberndof Professor in Healthcare Technology. As with actual COVID-19 patients, a lifelike simulator can depict rapidly decreasing oxygen levels, requiring teams to urgently don multiple layers of personal protective equipment, or PPE. Newly created devices, such as clear protective barriers, are now being tested and refined using simulation, she said.
“The main goal is preparedness,” Patterson said. “It’s about preparing the team to be ready and safe and to take care of the patient effectively and efficiently.”
The simulation team is made up of experts in health care, education and simulation operations who use innovative techniques and real-life, fast-changing scenarios to provide the opportunity for clinical experience in a risk-free environment.
Normally, they run simulations in the UF Health Shands Experiential Learning Center on the fourth floor of the George T. Harrell, M.D., Medical Education Building. But amid the COVID-19 pandemic, the team is running simulations within intensive care units and emergency rooms. Such simulations in an actual emergency room bay or ICU bedside are known as “in situ simulation,” and they elevate the realism and better represent the actual clinical scenario.
“We’re working in the environments where health care workers will be caring for patients, with the resources and equipment they usually have,” said Patterson, who directs simulation-based training and assessment across UF. “The muscle memory that people are learning, they’re going to be using it in this setting.”
Together with the leaders of each unit — the adult emergency room, pediatric emergency room, medical ICU, pediatric ICU and neuro ICU — the simulation team reviews specific needs, challenges and goals. After the simulation, the team then delivers a report to clinical leadership, highlighting potential safety threats and opportunities for improvement. Additional clinical units are also requesting simulations.
Simulations allow for testing and practice of newly developed COVID-19-specific approaches. For example, UF Health anesthesiologists Cameron Smith, M.D., Ph.D., and Nikolaus Gravenstein, M.D., working with UF engineers, have devised a new process using a transparent plastic drape to minimize viral spread during high-risk, aerosol-generating procedures such as intubation. Prior to implementation, ER and ICU teams are using the draping process in simulations, ensuring that any missteps occur on a manikin rather than a real patient.
UF Health emergency medicine physician Lars Beattie, M.D., said with COVID-19, draping is among other essential, specific procedures: Intubating a COVID-19 patient requires using a different approach to inserting the breathing tube. It involves rigorous planning and practice to ensure the safety of providers and to minimize the contamination of equipment. All health care workers in the room must wear additional layers of PPE, which increases the number of steps in the procedure and its complexity.
“Simulations allow us to identify specific ways to improve upon our process,” said Beattie, an associate professor of emergency medicine and residency program director. “It’s so essential for us to be able to get our heads around what’s different, what we need to think about, and establish our priorities.
In the UF Health Shands ERs and ICUs, teams of physicians, physician assistants, respiratory therapists, nurse practitioners, nurses and technicians are running and observing simulations, timing how quickly the team can don PPE and intubate a manikin mimicking severe COVID-19.
“The purpose of this training is to look at how we can refine technique,” said UF Health neurologist Marc-Alain Babi, M.D., program director of the neurocritical care fellowship who is helping lead simulations in the neuro ICU. “The team dynamic is extremely important for this high-risk procedure. There is a need for protocol and a strategic plan.”
Adherence to new Centers for Disease Control and Prevention guidelines created specifically for confirmed or suspected COVID-19 has required a swift change in mindset.
“We all have it ingrained that we just run into the room,” said UF Health pediatric ICU physician Jennifer Muñoz Pareja, M.D. “You have to practice and practice — it’s your heart and your mind that want to go into the room to help out. It’s a change in culture, a change in muscle memory. Now the mental model that all health care workers have is protect yourself first and then go into the room.”
She said health care workers facing the pandemic are putting into practice knowledge gained from experiences at other medical centers in hard-hit regions of the country and world.
“Every time you do this, there are new ideas of how to do it better,” said Muñoz Pareja, an assistant professor of pediatric critical care and pediatric critical care fellowship program director. “Everybody has learned a lot from New York, from Seattle, and we’re very lucky to have all that knowledge from those experiences and be able to implement them.”
Simulations help UF clinicians apply and test this knowledge, ensuring that patients experience the highest, safest level of care possible.
Learn more about UF Health’s efforts to combat the COVID-19 pandemic at Coronavirus.UFHealth.org.
Michelle Koidin Jaffee is the assistant director of communications for the McKnight Brain Institute of the University of Florida
Suggested Articles
No related articles found.



