
A 79-year-old patient with underlying health issues who was showing symptoms for COVID-19 was taken to a North Florida Regional Medical Center freestanding ER in Jonesville at 10 p.m. on March 18th.
At the time, the list of screening questions asked at the door of the ER facility were: Do you have a fever and cough/shortness of breath now or within the past 7 days?, Have you traveled in the geographic areas China, Iran, Italy, Japan, South Korea within the 14 days of symptom onset?, Have you had close contact with a laboratory-confirmed COVID-19 patient within 14 days?

A sample was taken for a COVID-19 test and sent to the nearest CDC location. The patient was transported via Alachua County Rescue to the hospital where she waited in the ICU for 8 days until she received the test result: negative.
A month later, a 53-year-old patient with underlying health issues exhibited four symptoms on an expanded list of testing criteria of COVID-19.
She called the Alachua County Health Department (352-334-8810) to see if she could get a COVID-19 test.

The expanded symptoms the FDOH representative asked about were fever, cough, shortness of breath, gastrointestinal issues such as diarrhea and possibly the loss of sense of smell or taste.
The patient also told the FDOH representative she was concerned about exposure because she lives with her husband who works at an essential retail store in Gainesville and he is exposed to the public and that she also cares for her 79-year-old mother.
The patient was directed by the FDOH to call her primary doctor and if a test was not prescribed, to then call the FDOH back for possible testing at a drive-thru testing site.
The 53-year-old patient called her primary physician and was scheduled for a telemedicine appointment via Zoom two hours later. From that consult, a test for COVID-19 was ordered by the physician. The patient received a phone call and scheduled that test at the UF Health Family Medicine-Springhill testing site.
Upon arrival at the Springhill facility off 39th Avenue there was one car in line and a drive-up testing site lit up and manned with several nurses. Further down in the parking structure, the patient counted 10 more testing sites sitting unused.
A nurse wearing a gown, face mask, protective face shield and gloves explained how the testing worked and directed the patient to pull up to a testing area where her ID was verified.
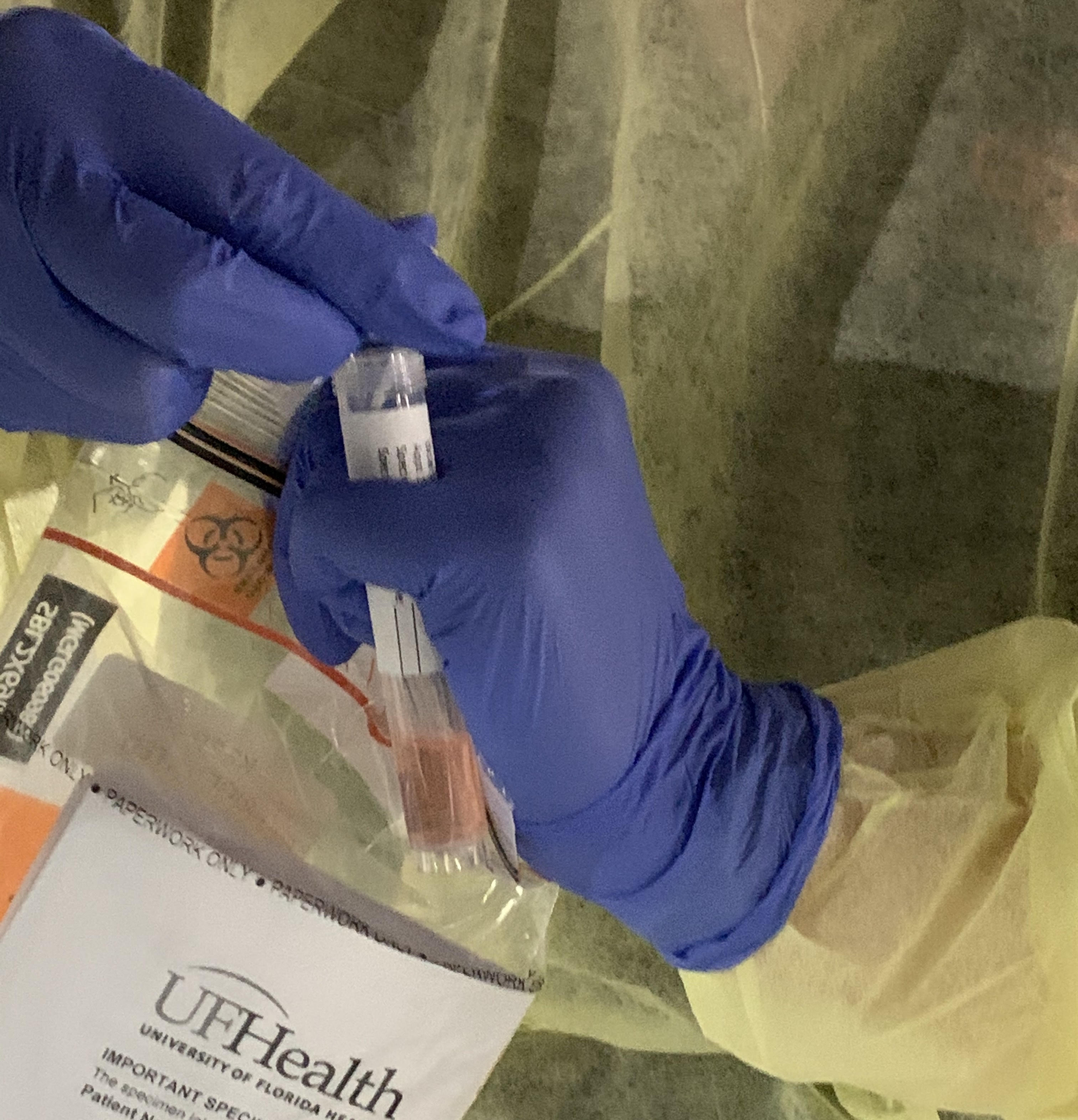
“It’s going to burn,” the nurse administering the test warned. And she was right. For the 10 seconds that it took to collect the sample it burned as the swab reached way back into the nasal cavity.
“I know, I’m sorry,” the nurse said, and told the patient that whoever ordered the test would be contacting the patient with the results. She handed the patient a “Viral Syndrome Home Discharge Sheet” that explained that the symptoms reported that lead to the order for the COVID-19 tests could be caused by an influenza virus, the common cold or possibly the COVID-19 virus.
“Most patients with COVID-19 infection have mild symptoms and recover on their own,” the sheet read. “Resting, staying hydrated, and sleeping are typically helpful. At this time, you are well enough to go home and treat your symptoms with oral fluids, medicines for fevers, cough, pain, etc. If your symptoms worsen you can always contact us for re-evaluation.”
The sheet also spelled out the CDC guidelines for minimizing spread of infection and how to self-isolate effectively.
The sheet closed with, “We wish you all the best and will remain a partner in your care. Remember, the overwhelming majority of people with viral flu symptoms, including COVID-19 infections, recover from their illness. By following the guidelines on these pages, you can help improve your recovery and decrease the risk of passing an infection on to others.”
The 53-year-old patient went home and followed those instructions.
Seven hours later she received a message via email in all caps that the CORONAVIRUS (COVID-19) was “Not Detected.”
Photos by Staff Photographer Suzette Cook
Suggested Articles
No related articles found.



