
Last March COVID-19 began appearing in North Florida. At UF Health Shands Hospital’s Unit 75, some doctors and nurses had a feeling of inevitability. Their unit had earned a reputation for expertise and teamwork — as well as being home to some of the hospital’s pilot projects.
Dr. Nila Radhakrishnan the division chief of hospital medicine, distinctly recalls one March day in the hospital’s Command Center. The first COVID-19 patients were being admitted. Among a group of leaders that included the hospital’s CEO and chief nursing officer, a question percolated.
“Everyone asked which unit should be the non-intensive care COVID-19 unit to start, and the answer was Unit 75 because of the proven track record of teamwork,” Radhakrishnan said.
For those working in Unit 75, a group of about 12 nurses per shift and two to five hospital physicians at a time, uncertainty was a given. None of them could know how much change was coming at work and at home — and how quickly. Infection control precautions interrupted their natural reflexes to rush at a patient in distress. The garb that provided crucial protection was uncomfortable, even stifling. For infection control, COVID-19 patients were allowed no visitors.
Yet, when the word came down, the front-line workers of Unit 75 never flinched. Hospital leadership ensured the unit was well-stocked with personal protective equipment. By the Christmas holidays, they were seasoned veterans of COVID-19 care. These front-line workers persisted in caring for the sickest patients even as the pandemic exploded again nationwide in the late fall.
“I had multiple physicians step up and tell me they wanted to care for COVID patients. Our nurses knew exactly what had to be done and that it wouldn’t be easy, but they did not hesitate,” Radhakrishnan said.
As the seasons changed, so did the COVID-19 dynamic. Colder weather and the winter holidays had experts expecting the virus to spread rapidly. Yet, there were always reasons for hope: A UF Health pediatrician served on a prominent national committee making key recommendations on how to prioritize the vaccines. On Dec. 16, the first COVID-19 vaccinations were given to UF Health’s front-line workers.
Across the UF campus, many people have worked tirelessly to defeat the pandemic and mitigate its effects. Hospital workers in units 74, 75, 82 and 94 have cared for many COVID-19 patients. Researchers have toiled over ways to exploit the virus’s vulnerabilities.
In the pandemic’s early days, scientists devised low-cost, open-source ventilators. An engineering professor worked with 3D printing experts to develop a massive supply of nasal swabs for COVID-19 testing. Epidemiologists and infectious disease experts developed Screen, Test & Protect protocols to foster a culture of care for the UF community while helping to prevent the spread of COVID-19.
This is a look at one part of that unprecedented effort, a glimpse into how teams assigned to ground zero at UF Health — Unit 75 — have battled COVID-19 for nearly a year and learned on the fly how to combat the novel coronavirus both at work and at home.

Safety drives patient-care changes
Nurses, doctors and other care providers are used to scrambling a big team when a hospital patient goes into “code blue” or cardiac arrest. For patients with COVID-19 — an airborne, potentially lethal virus — new, unique responses were developed immediately.
Protective gear needed to be donned quickly but perfectly. A charge nurse was assigned to make sure that happened. Routine protocols had to be revised to address how many caregivers can be in a COVID-19 patient’s room during a cardiac arrest.
“It’s a high-stress environment even without COVID,’’ Radhakrishnan said. “Your patient is dying because their heart or lungs have stopped. Usually, all of us just drop what we’re doing and run in. But you can’t do that with COVID patients.’’
Myriad other considerations for working in a COVID-19 environment emerged, she said. Performing CPR on a patient generates airborne particles. Starting ventilator treatment means inserting a tube in the patient’s throat. To practice for these events, the critical care team, simulation team and nursing teams worked together to stage “mock codes.”
Plastic curtains were placed across doorways, allowing unit staff to hear what was happening during an emergency without entering the patient’s room.
With everyone shrouded in protective gear, even the simple task of recognizing colleagues became a challenge. The solution: handmade tags identifying the co-workers. R.N. Physician. Respiratory therapist. Charge nurse.
“We knew that we couldn’t have 10 people at once in a patient’s room,” Radhakrishnan said. “You don’t always know right away who is in the room with you, so the tags let everyone know you have a nurse and the physician.”
To preserve protective equipment, hospitalists were the only physicians going into COVID-19 patients’ rooms. The patients’ other doctors called in or did consults electronically.
The elaborate protective gear created another unexpected dynamic.
“The family members who would ordinarily support a patient aren’t there. Then, we all arrive covered in protective gear. Sometimes, we couldn’t help but get to the patients and lay hands on them, sit next to them,” Radhakrishnan said.
“We, as hospitalists, were trying to provide all of our empathy and compassion but it wasn’t always up to the level that we could have achieved. The nurses picked up on that and made up for that gap,” she said.
That kind of dedication is remarkable, UF Health Shands CEO Ed Jimenez said.
“In this unprecedented time for health care workers, our patient-care teams have done more than just meet the challenges of the COVID-19 pandemic,” he said. “Every day for many months, they have given their time, energy and spirit to assure that our patients have the best care possible – and they continue to do so. I am profoundly grateful and deeply touched by the determination and compassion that is shown every day.”
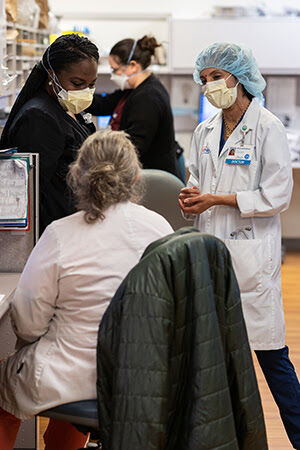
For front-line workers, COVID-19 hits home
The uncertainty and fear related to the virus followed the Unit 75 team members home.
“Among some physicians, there was a lot of concern,” Radhakrishnan said. “Even now, I know doctors who are staying separated from their families. I had people wondering out loud, ‘Should I hug my children?’
Sapheria Pollard, R.N., the clinical leader for Unit 75, has a 3-year-old son but chose not to isolate herself from him in the pandemic’s early days. Still, her job brought lifestyle concessions large and small. She doesn’t drive home in her work shoes. They go straight into a bin in her car trunk. When cases spiked in March, Pollard didn’t see her out-of-town relatives for months. Her significant other, who also works in health care, was exposed to COVID-19 on the job.
Beth Digao, R.N., a Unit 75 nurse, and her husband were tested twice for COVID-19 because a relative needed to quarantine. Working in a COVID-19 environment and also taking precautions outside of work is about being vigilant and detail-oriented: The constant use of hand sanitizer. Putting on and taking off protective equipment the right way.
“It was concerning at first, especially when we were told we would be the COVID unit. As a nurse, you don’t just worry about yourself. You worry about your patients. You worry about your family. But we learned to adapt and told each other that we can do this,” Digao said.
The extensive precautions have proved to be effective. None of the hospital physicians have contracted COVID-19 from working in the unit. Patients have also fared better: Through early January, the COVID-19 death rate at UF Health remained significantly below the national average — something Radhakrishnan and others are trying to better understand with research into UF Health’s approach to early rescue of patients and patient outcomes.
For the unit’s doctors and nurses, COVID-19 precautions have also posed emotional challenges.
Pollard often makes rounds to see if patients are interested in doing Zoom calls with relatives. She makes sure they know about puzzle books, coloring books and opportunities to paint on a canvas. Pollard has seen patients light up when handmade cards with encouraging messages written by caring strangers show up.
“We try to give them a little piece of home — especially with the Zoom calls,” she said.
The front-line workers also have a legion of supporters behind them. Two third-year UF medical students organized Gator Sitters, a team of medical and physician assistant students who volunteer their time to provide child care, pet care and other household help such as meal preparation and grocery shopping.
At Thanksgiving, a group of Eastside High School students created more than 50 handwritten cards expressing their gratitude to UF Health doctors and nurses. They also produced a video thanking front-line workers who have carried on throughout the pandemic.
It’s all been a lot to handle, but Pollard and her co-workers persevered. In the spring, nurses said they were exhausted because they didn’t know what to expect. Now, Pollard said they feel fatigued more than anything. Just when it seemed COVID-19 cases might start falling, they picked back up.
“We would like to think the vaccine is the light at the end of the tunnel,” Pollard said. “But we know it will take time to see the impact.”
Exhaustion and optimism
COVID-19 has even altered the most intimate, challenging conversations doctors have with their patients. A troubling new diagnosis or end-of-life conversation normally happens with the patient, their family, the doctor, a nurse and a palliative care specialist. Contagion now makes that in-person discussion difficult.
Seeing COVID-19 patients die alone has been profoundly difficult for many physicians and nurses. “That has been the most emotionally exhausting part of providing their care,” Radhakrishnan said.
To help with end-of-life care, the nurses have been especially helpful in making exceptions to the visitor policy. The palliative care team has helped with end-of-life discussions.
The mix of draining experiences and successful outcomes are also what propels her team forward. As division chief of hospital medicine, she assigned some physicians fewer COVID-19 patients. That assures they have the time and emotional energy to spend with families and patients when difficult decisions arise.
There are also reasons for optimism: A UF Health pediatrician, Dr. Sonja Rasmussen, was part of a prestigious national committee that made key recommendations to federal officials on how the vaccines should be allocated. COVID-19 vaccines are being administered at UF Health and in the community. Across the UF campus, many COVID-19 research projects are continuing apace.
Radhakrishnan said she is heartened by the vaccines’ safety and efficacy. She also sees hope in the potential for herd immunity and the enduring resolve of her colleagues.
“We are indebted to each and every person who has helped with COVID-19 care. It is clear that there are many unsung heroes who, right at this moment, are contributing to compassionate care,” she said.
For every challenge on Unit 75, there have been many successes. Most patients get better and go home. Digao, a Unit 75 nurse, said there is nothing more rewarding.
“When we bring patients downstairs and see them meet their family, we’re just so thrilled to see them go home,” she said.
For Radhakrishnan, watching her team care for COVID-19 patients affirmed what she already knew: Everyone including nurses, physical therapists, speech and swallowing experts and environmental services workers saw the special challenges and rose to meet them. Pollard watched nurses deliver food trays and transport patients — tasks that would be done by other workers in a less-contagious environment.
“You work as a team,” Pollard said. “There is no other option.”
Suggested Articles
No related articles found.



