The scenes that Gainesville RN Lori Smith describes in New York sound as though she was on the frontlines of a battlefield.
“You can see fear in the eyes of those that are still maintaining their oxygen levels above 90 percent,” Smith says about the COVID-19 patients she is serving at a hospital in North Central Bronx.
“And those that drop below become so confused they become their own worst enemy. Constantly removing their oxygen masks, and trying to get out of bed making their shortness of breath worse. We try to tell them, ‘if you keep taking this off you are going to die, you have to have this oxygen’ but their confusion gets so bad they aren’t able to understand any direction at that point.”

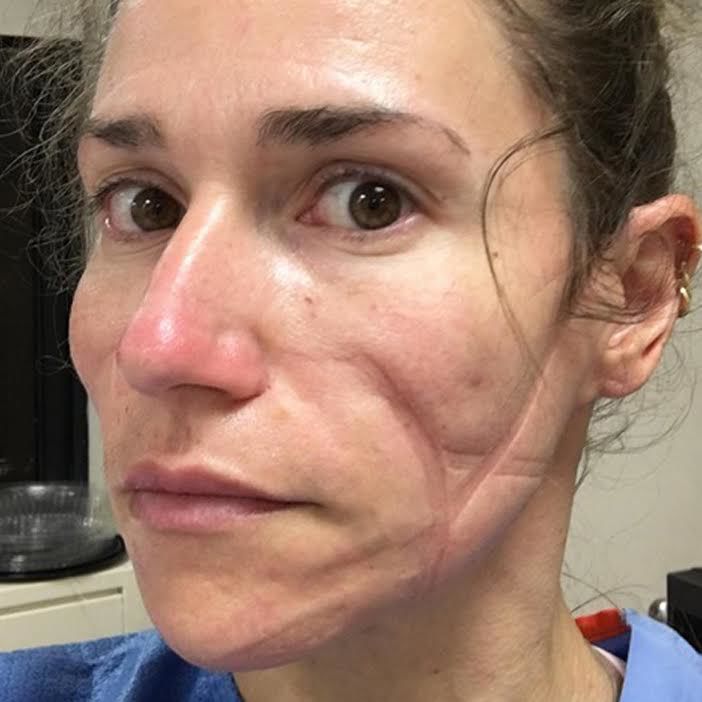
In a selfie photo taken upon arrival in New York City, the epicenter of the global pandemic that has claimed more than 70,590 victims globally and more than 9,654 in the U.S. as of noon on April 6, Smith and her coworkers are smiling. A week later, Smith’s selfie reveals the emotional and physical toll her 21-day assignment to a medical surgical floor is taking. There are deep gouge marks on her face made by a fitted N95 face mask, and the smile is gone.
“I’m lucky if I can get five hours of sleep a night,” says Smith, 38, who works at UF Health Shands Endoscopy and Adult ER Departments.
“I was originally assigned to the ER and that is the experience I have,” Smith says. “But the ER at this facility did not want outside nurses down there (getting in their way), so I got reassigned.”
“I was disappointed at first because I felt that my experience could be used better elsewhere, but I reminded myself that I promised to help in any way they needed me.
“Then I got to the floor and it was really sad. My first shift there were only two staff nurses for 27 patients, so when they brought three extra travel nurses onto the unit, it was like a miracle had just occurred for them.”
When Smith arrived to begin her first 7 p.m. to 7 a.m. shift, there were 18 patients who were COVID-19 positive, six were COVID-19 rule outs (which means testing is pending but will likely be positive), and three patients with other diagnosis.
“The rule-out patients are put in the same room with each other because there aren’t enough areas to keep everyone isolated,” Smith says. “So unfortunately, if one person was negative and their roommate ends up positive, they are both positive now. All of COVID patients are on oxygen and still have difficulties maintaining their oxygen levels.
“I notified a doctor last night that a patient was on the maximum amount of oxygen we can give and his saturation was at 88 percent. He looked at me and said, ‘I can’t do anything about it, let me know when he drops below 82 percent and we’ll intubate him.’
“I know that the situation is extreme now, but I feel like all of these patients are just waiting until they get bad enough that they need intubation and then will most likely die.”
Smith can attest to the dwindling supply of personal protective equipment that is discussed daily during coronavirus briefings on the national news.
“I’ve already been informed that for tonight’s shift we will no longer be receiving disposable paper scrubs.” She says. “I have been reusing the same N95 mask.
“I was told I could get a new one every week. We will see when my first week is over if that happens or not. The heat from breathing in your own air all shift from wearing a mask makes my nose run and drip into my mask, so I am praying that doesn’t compromise the integrity of it.
“There aren’t enough ventilators because they are now triaging when to put someone on a vent. The standards for venting someone have dropped considerably. My patient last night at 88 percent would have been intubated in a normal situation.”
Smith says she has not worked the night shift before. “I had one day to adjust,” she says.
“We are bused from our hotel to the hospital and during loading and unloading of the bus, people walking by in the streets applaud and thank us for ‘our service.’
“At the start of shift everything is chaotic, but we are just starting so we have energy. Wearing masks muffles your speech so it is difficult to hear and communicate.
“That leads to frustration as the shift goes on and you get tired of not being heard and having to repeat yourself over as over again. Wearing the N95 decreases your oxygenation because you are breathing in your own CO2 constantly, which leads to a headache,” Smith says.
“The headache for me starts about two hours into shift and only gets worse throughout. By eight hours into the shift my thought process slows down and it becomes really hard to concentrate. After a full 12-hour shift, I have severe detentions on my face from wearing the mask, my ears hurt, my head is splitting, and my nose feels like I’ve been punched dead on.
“But at the end of shift, the staff nurses express their gratitude for our help. And I remember that at anytime I can leave and don’t have to put up with this anymore, but the staff here can’t. This is their home and they will drown without help.”
Smith, who lives in Newberry, wants Floridians to know that the seriousness of this pandemic is real. “This virus is highly contagious and there are healthy young people dying also,” she says. “Treat the mandatory self quarantine like a way to save your life. Things are going to get worse before they get better.
“Of course I have a concern about my own health,” Smith says. “Before I left, I cried thinking about the worst-case scenario and made sure I went over my end-of-life desires and life insurance with my husband. He reminded me that I didn’t have to do this. And I told him, ‘I’m a nurse! I’ve been at home for a week not needed by my facility. I can’t in good conscious continue staying at home when distress calls are going off. I need to go.’”
To protect her health, Smith says she is committed to proper isolation techniques. “I wash my hands frequently, wear my mask and hope that if I contract the virus, I am one that will be asymptomatic and then properly isolate myself.
“One of my co-workers here was on a floor our first night working beside a staff nurse that fell out mid shift and they had to intubate her on the ground. That’s a really scary possibility that I can only pray doesn’t happen to me.”
When Smith returns to Gainesville from New York she will be in quarantine for 14 days before she can work again. As of noon on April 6th, Alachua County had 123 positive cases of COVID-19 reported and Florida had 13,325 with a concentration of that total in Miami/Dade County with 4,146.
“It’s still a little early to state what I have learned with conviction,” Smith says. “But one thing is certain. We MUST protect the healthcare workers. All of the ventilators in the world will not do any good if you don’t have the staff to manage them. There is an alarming rate of healthcare workers here that are falling sick.
“The problem with the ventilators isn’t just about having enough ventilators,” she adds. “It’s about having enough staff to continue management of them.
“You can’t win a war if you send your soldiers to battle without armor.”
To read part four: “Gainesville nurse resigns to answer calling in New York City hospital”, go here.
This is the third in a series entitled “Frontline NYC” by Mainstreet Daily News Staff Writer Suzette Cook about the experiences of nurses from Gainesville dispatched to New York City in the fight against COVID-19.
Suggested Articles
No related articles found.



