
University of Florida Health recently enrolled the first two patients in a national study examining whether convalescent blood plasma can stop the progression of COVID-19 from a mild to severe form of the disease in patients with relatively minor symptoms.
The study, Clinical Trial of COVID-19 Convalescent Plasma of Outpatients, or C3PO, involves 50 medical centers and is a blinded, placebo controlled, randomized trial that expects to enroll 600 participants. Half will receive convalescent blood plasma and the rest a multivitamin in a saline solution.
Blinded means patients do not know if they received the placebo or the blood plasma.
Enrolled patients must have a mild form of COVID-19, the disease caused by the coronavirus, that does not require hospitalization, said Lisa H. Merck, M.D., M.P.H., an associate professor who is vice chair of research in the UF College of Medicine’s department of emergency medicine and site principal investigator of C3PO at UF Health.
She said the trial’s participants also must have one of several risk factors that make them more susceptible to a severe case of COVID-19. Those include being over age 50, having heart or lung disease or diabetes, or being immunocompromised.
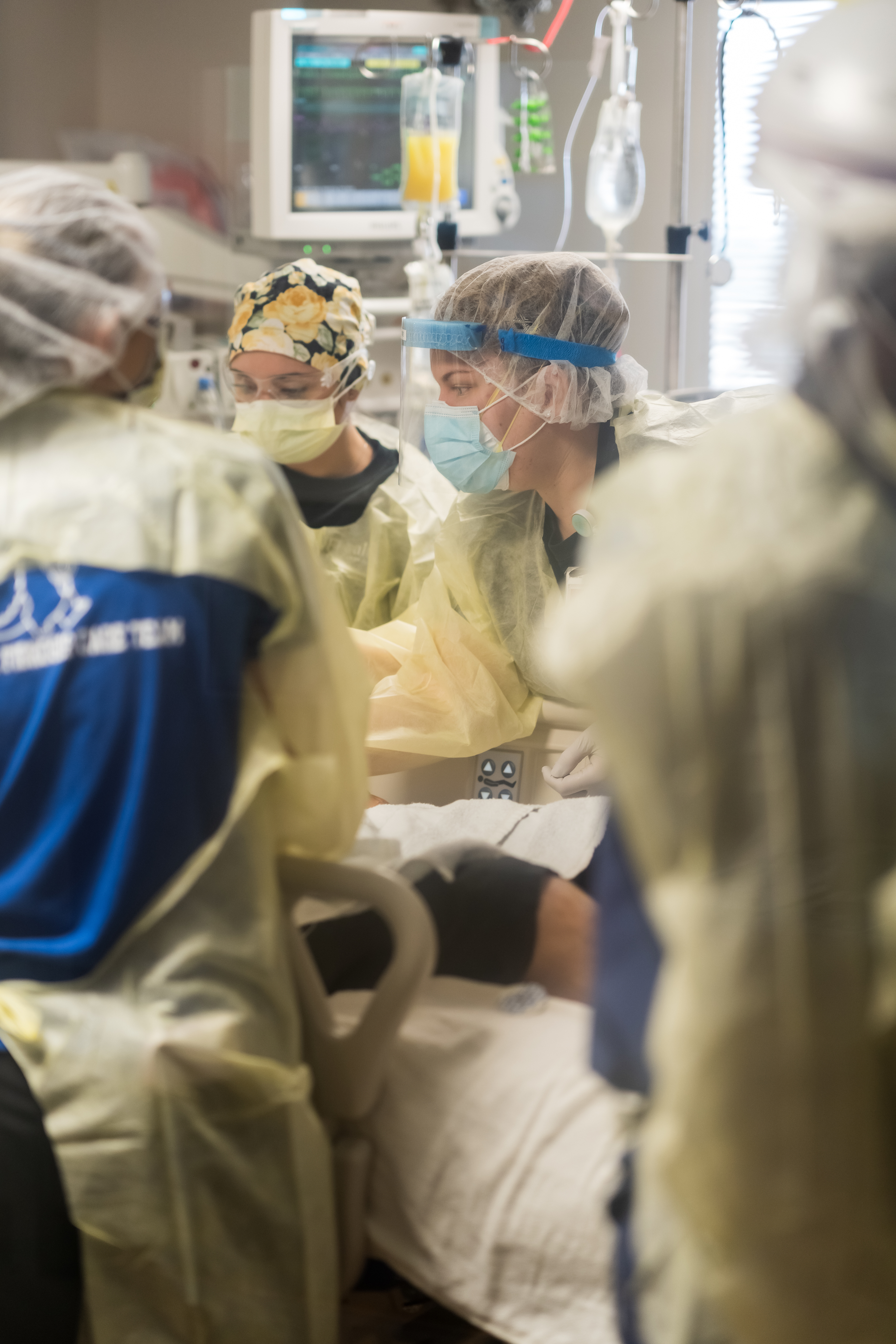
These are patients seen in emergency rooms such as the one at UF Health Shands Hospital. If the patients provide their consent, they will receive an infusion of either convalescent blood plasma or placebo.
“We are trying to see if the blood plasma gives these patients an edge in the outpatient environment — if the antibodies from the plasma give them the extra boost to fight the virus,” said Merck. “This is a study that could ultimately change how we treat this population of patients.”
The U.S. Food and Drug Administration recently granted emergency use authorization for convalescent plasma in hospitalized patients. That decision does not have an impact on the current study, which involves patients early in the course of illness, who are discharged from emergency rooms.
Convalescent plasma is an old concept in medicine. First used in 1892 with the bacterial infection diphtheria, the therapy played a role in the Spanish flu pandemic of 1918, and more recently was administered during the Ebola and the H1N1 flu outbreaks, among others.
Until now, no national randomized control trial, the gold standard of clinical research, has tested convalescent plasma’s efficacy.
Plasma is the liquid part of the blood. Light yellow in color, it’s mostly water, accounting for about half of a person’s blood. The rest is red and white blood cells and platelets. Most importantly, blood plasma contains the antibodies that fight disease.
The body produces antibodies when exposed to a foreign pathogen. Antibodies, which are proteins, bind to viral invaders and deactivate them. As a result, the invaders don’t get the chance to infiltrate and damage cells.
When a person recovers from illness, the antibodies remain for a period of time.
If someone receives a vaccine against an illness, it will take them some time to build up antibody levels in their blood. This is known as active immunity. By infusing a sick person with the blood plasma of someone who has recovered, passive immunity might be conferred much more quickly.
J. Peter Pelletier, M.D., medical director of the UF Health Shands Blood Bank and a co-principal investigator of the C3PO at UF Health, said medical centers around the nation have mostly been using convalescent plasma as a therapy of last resort with the most critically ill patients.
The C3PO study is focusing on the use of convalescent plasma, collected by blood banks, that has a high load of antibodies.
Study participants will be tracked for a month, although researchers are focused on the first two weeks, when the course of a patient’s illness begins to become more defined, Pelletier said.
Kartik Cherabuddi, M.D., an associate professor in the UF College of Medicine’s division of infectious diseases and global medicine and the director of the antimicrobial management program at UF Health, said it makes sense to assess the use of convalescent plasma early in the disease’s progression.
“The viral phase of the illness is completed in the first eight, nine or 10 days,” he said. “People on the ventilator are usually in the post-viral phase. If you use convalescent plasma in that situation, it likely affords very little benefit. That’s why this trial is so important. It addresses the right population. You’re likely to get the most important benefit with this group, if there is a benefit.”
Merck said UF Health’s involvement in C3PO has received important support from UF Health Shands Chief Information Officer Gigi Lipori, M.T., M.B.A., in addition to UF Health’s IT and integrated data repository teams. Merck said they did an “incredible job” helping initiate the trial here.
“We had to ensure the enrollment could begin the moment UF received approvals from the national coordinating center,” said Lipori, a co-investigator of C3PO. “The level of collaboration and commitment involved to advance critical research during a pandemic, along with the complex challenges that occur every day at an academic health center, is truly incredible.”
Merck noted C3PO is one piece of the COVID-19 puzzle and that UF Health researchers are working on numerous efforts to counter the coronavirus.
“The landscape for COVID-19 — our understanding of how the coronavirus manifests in different patients — is being defined daily,” she said. “It’s exciting that UF Health personnel, from the basic science labs to the ICUs, are working nonstop to improve care for patients.”
C3PO is coordinated through The Strategies to Innovate Emergency Care Clinical Trials Network, or SIREN. This National Institutes of Health-funded effort seeks to improve outcomes of patients with neurologic, cardiac, respiratory, hematologic and trauma emergencies by identifying effective treatments administered in the earliest stages of critical care. The UF College of Medicine’s department of emergency medicine is one of 11 hubs for research within SIREN.
C3PO is supported by the National Heart, Lung and Blood Institute in collaboration with the Biomedical Advanced Research and Development Authority. Research is led by investigators at the University of Michigan, the University of Pittsburgh, the Medical University of South Carolina and Stanford Medicine.
Visit https://siren.network/clinical-trials/c3po for more information.
Suggested Articles
No related articles found.



