My husband is lounging on St. Augustine Beach, soaking in the sun and tuning out stress while he rests. His eyes are closed as he listens to the sound of the waves.
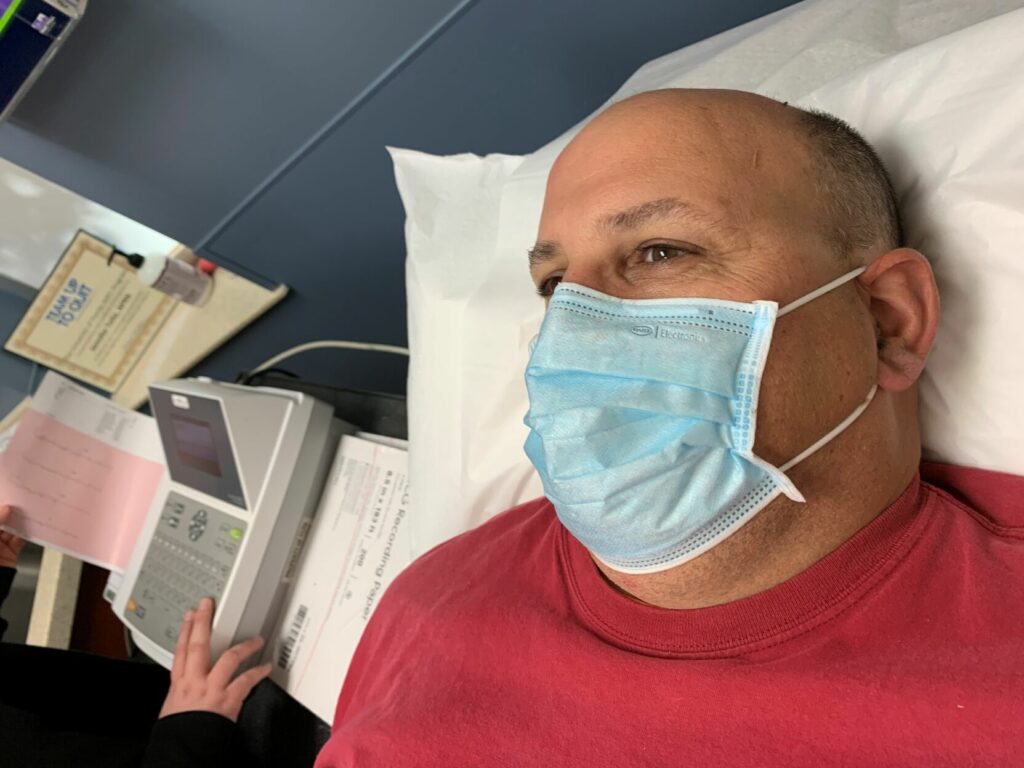
The day before, he was hooked up to an EkG machine and having bloodwork ordered for a D-dimer test that can detect an embolism caused by a blood clot. If negative, his doctor said he can hold off on the very expensive CT heart scan.
He is three weeks post COVID-19, but far from back to normal as he experiences a racing heart and tightness in his chest. And as we navigate the post-COVID-19 experience, here are some discoveries we have made that might help others who are on this journey too.
Before the pandemic, my husband Aaron, 49, never called out sick from work. No colds, no flu, and always super active—from running around Disney every week to swimming and kayaking local rivers. But then COVID-19 came and he missed three weeks of work. Now he’s doing half days on his doctor’s orders.
He is lucky to not have spent time in an ICU, but, at its worst, COVID-19 sent him to the ER with difficulty breathing and a heart that often beat past 100 beats per minute at rest. I was luckier than my husband just experiencing gastric problems, fatigue, and loss of taste, so I am back to normal since testing negative two weeks ago.
Studies have documented that COVID-19 can damage the heart, blood vessels, kidneys, brain, skin, eyes, and gastrointestinal organs. Many patients refer to having a brain fog afterward that affects their thought process and memory.
The CDC reports that more than 90 percent of people with the flu recover within two weeks of a positive test. But with COVID-19, all bets are off.
According to the CDC, the most commonly reported long-term post COVID-19 symptoms include: fatigue, shortness of breath, cough, joint pain, and chest pain. Other reported long-term symptoms include: difficulty with thinking and concentration (sometimes referred to as brain fog), depression, muscle pain, headache, intermittent fever, and fast-beating or pounding heart, also known as heart palpitations. My husband is experiencing all of these.
Our biggest concern is the toll the virus has taken on his cardiovascular, neurological systems and on his mind. We know it will take a team of specialists to access Aaron’s condition and put him on the path to recovery that is tailored to his situation. There is a balance we are looking for between getting back to work and normal life but not pushing too hard and preventing him from recharging and healing.
UF Health has been moving us in the right direction, but there are several Post Covid Care Centers (PCCC) now established in Florida that are ahead of the curve when it comes to the team approach to righting the damage COVID-19 can do to the body.
According to Survivor Corps website, The Watson Clinic Post COVID-19 Clinic in Lakeland provides a comprehensive evaluation, offers lab tests, pulmonary function tests, radiology evaluations and other tests designed to detect depression, cognitive ability, physical maladies, nutritional deficiencies and neurological disorders. The clinic then provides treatment intended to get survivors back to a pre-COVID quality of life. To make an appointment: Call 863-680-7190.
In Miami, the heart experts at the University of Miami Health System have established a special program to address health issues related to heart inflammation and scarring due to COVID-19 infections and untreated heart problems. Call (305) 243-2788 to make an appointment.
In Tampa, the COVID Confirmed (COCO) Clinic at the Global Emerging Diseases Institute at Tampa Health is run by infectious disease physicians from the Department of Internal Medicine at USF Health, Morsani College of Medicine. It runs in partnership with Tampa General Hospital and the Florida Department of Health.
The COCO Clinic offers a comprehensive network of healthcare professionals who are committed to providing specialized care for patients who have tested positive for COVID-19. The clinic will virtually provide complete health assessments, track patients’ symptoms and provide expert advice and medical instruction so that patients can safely manage their COVID symptoms at home. If required, in-patient care may also be provided. An emphasis will be put on taking care of COVID-19 Long Haulers, those survivors who continue to have side effects weeks, or months, after being considered “recovered.” Call (813) 974-7616 to be directed to the COCO Clinic.
Information about these PCCCS can be found on this website and there is a map of the U.S. where you can find other PCCCs from coast to coast by clicking on the state you want to learn about.
We chose the PCCC that best fit Aaron’s situation and scheduled a telemed visit and plan to lock in a team that we hope will not only expedite his healing in a safe way but use the data from his diagnostics to help the thousands of long haulers who will continue to follow in Aaron’s footsteps.
To see the beginning of our journey visit the first story in this series that documents our battle and recovery from COVID-19.
Suggested Articles
No related articles found.



