
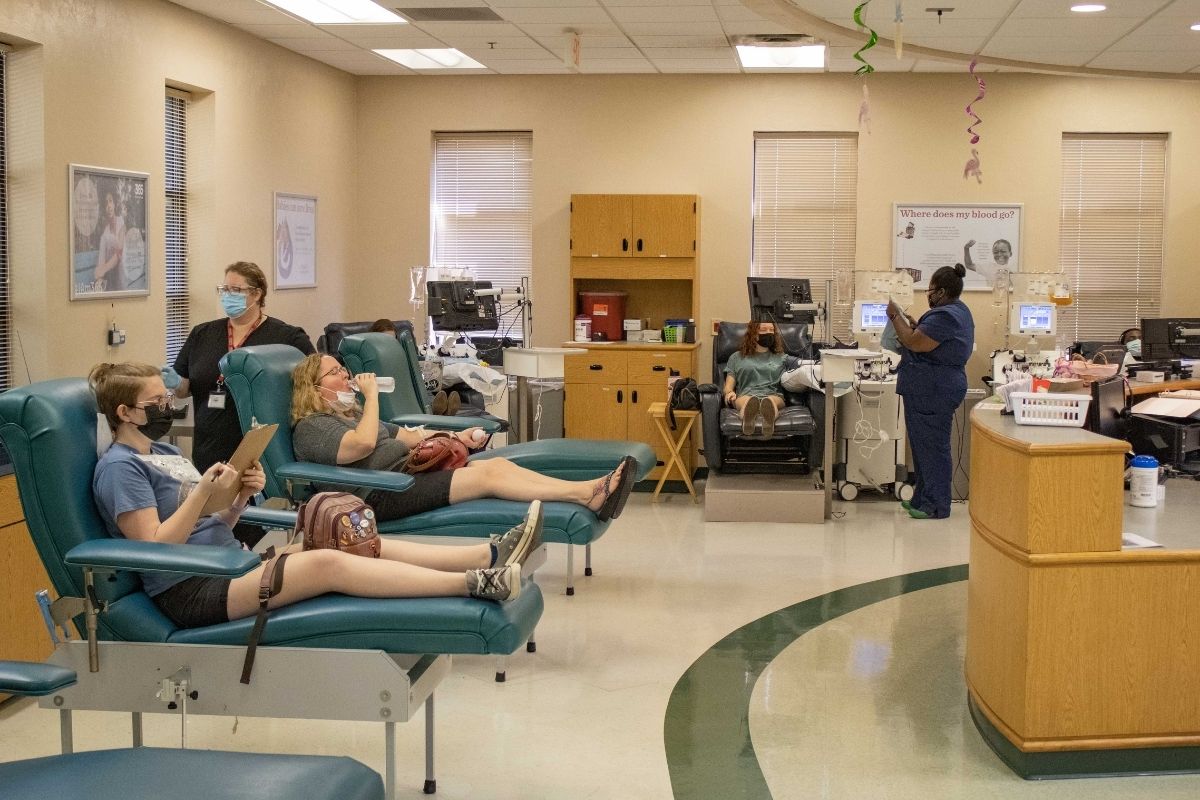
Blood donation requires multiple steps, checks and pieces of specialized equipment. Donors can probably guess some of the supplies—needles, centrifuges and snacks.
Other equipment, like cookie sheets, might be unexpected.
LifeSouth Community Blood Centers provides the majority of blood to area hospitals like UF Health Shands or HCA Florida North Florida Hospital.
At LifeSouth’s centers or mobile events, the clock starts ticking once blood leaves a donor. LifeSouth has eight hours to put it on ice and has a variety of ways to use the blood.
Depending on the current needs, the blood could stay whole with all the plasma, platelets and cells kept in one unit. Or LifeSouth might separate the components to make units of pure platelets, plasma or red blood cells.
Dr. Joseph Peter R. Pelletier oversees transfusion services at UF Health. He says separating blood maximizes donations.
“If we were to give the whole blood right away, patients may not need parts of those components,” Pelletier said in a phone interview.

LifeSouth Donation Center on Newberry Road.
He explains that an anemic patient without coagulopathy (clotting ability) only needs red cells. If a patient’s platelet count is low but they aren’t anemic or coagulopathic, the patient just needs platelets—not the red cells or plasma.
“So we give them the component that’s specific to their needs,” Pelletier said.
This process allows one blood donor to provide units for up to four patients.
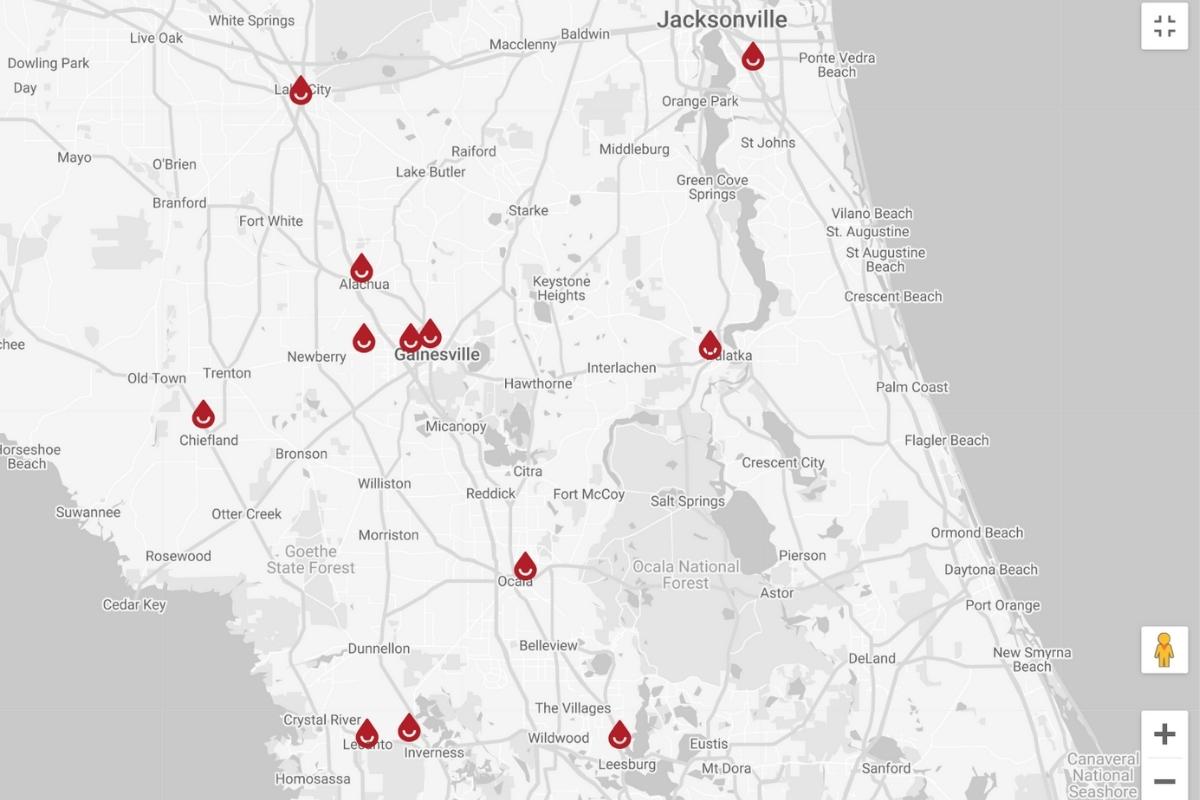
No matter the product LifeSouth plans to make, all donations given within Florida arrive in Gainesville for processing off of NW 13th Street, just a few blocks south of Gainesville High School.
LifeSouth has centers throughout Alachua County and in Lake City, Palatka, Jacksonville, Chiefland, Ocala and further south.
Once in Gainesville, employees decide what product to make based on the type of blood and current needs.
The processing room contains a mix of old and new equipment and stays at a cool temperature. In one corner, bags of plasma soak in a tub of moving water as workers with latex gloves move between stations.
Kevin Jenkins, regional manager at LifeSouth, said the room just added another AC unit to battle against the centrifuges, fridges and freezers constantly putting out heat.
The production process contains a host of checks. The room temperature is continually monitored along with each fridge and freezer. All the centrifuges have diagnostics run in the morning, and a host of barcodes track each donation and the separate parts made from the blood.
First, blood units get weighed and many units get sent to centrifuges to separate the components.
While spinning at thousands of revolutions per minute, the denser red blood cells group on the bottom while the plasma floats. Then employees place the products into separate bags, either manually or by using an automatic machine.
The cost of processing blood depends on the end products. Jenkins said hospitals love the pathogen-reduced cryo because, once thawed, it has a longer shelf life compared to just pathogen-reduced units—from a matter of hours to five days.
He said that advantage comes with a good-sized bump in the production cost. New equipment also comes with a higher price tag.
The tool employees use post-centrifuge to separate components costs less than $1,000. The new automatic machines come in at $30,000. And the new German freezer costs around double the old one.
Once processed, products get frozen for storage. That’s where the cookie sheets come in. Jenkins said the company needed a name for the flat, metal pans that slide in and out of the freezer. Given the similar look, LifeSouth adopted cookie sheets as the name.
LifeSouth sends samples of the blood for testing in Atlanta. The lab checks for abnormalities within the products and typically gives the green light in 18 hours.
Machines within the processing center also analyze plasma samples for anything amiss. Jenkins said FDA requirements changed recently, mandating two samples per unit.
The requirement takes longer and limits LifeSouth’s processing quantity so the company purchased an additional machine to bring capacity to 1,200 vials of plasma.
The machines rocks the vials back and forth while searching for anything growing. If the machines find something, it sends an alert.
Jenkins said the machines give more false positives than not. Since January, LifeSouth has received three real alerts and roughly 12 false positives.
He said a little dandruff might enter the machine and trigger the alert. Or keeping the machine open longer than normal could also set it off.
Distribution-ready units enter a walk-in fridge that divides the room. On the distribution side, a TV monitor tracks the requests coming in from hospitals.
Recently, LifeSouth has faced donor shortages, and blood centers across the nation have hovered at one or two day supply.
On a low day, Jenkins said the processing center could get 60 units from across Florida while high days bring in around 200. He said the center would like around 150 daily units to keep its levels secure.
At UF Health, the blood units come in and out without much pause.
“We get resupplied at least twice a day with blood, so it doesn’t stay around long once it gets here,” Pelletier said.
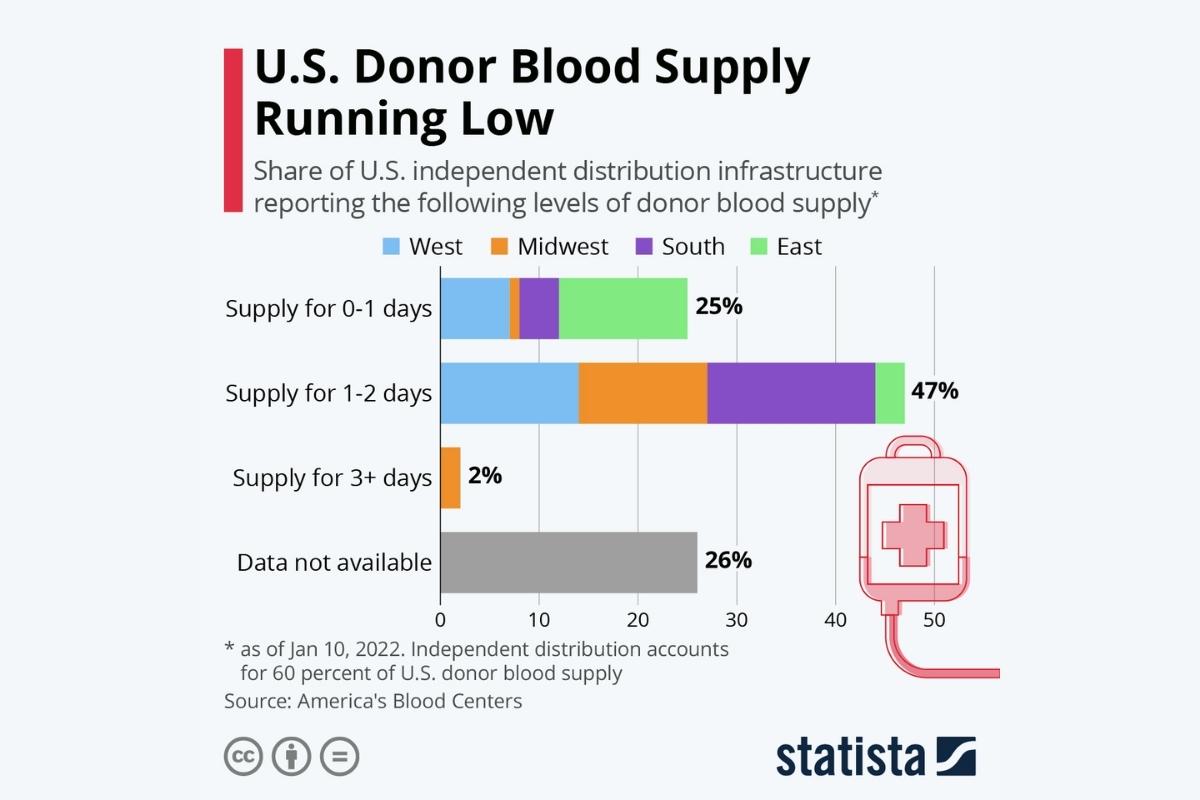
An O type shortage has affected the county over the past six months, Pelletier said, and UF Health and LifeSouth have begun to feel those effects within the past month and a half. He said they’ve never had an O type shortage.
UF Health contains several programs that need a lot of blood: allogeneic stem cells, allogeneic bone marrow transplants, solid organ transplants, burn units and a Level I trauma center for both adults and pediatrics.
The top-rated trauma center means UF Health could require a sudden increase in whole blood units.
Jenkins said that happened a few weeks ago when a semi truck hit a school bus in Levy County. The processing center received an alert for more than 45 units of whole blood, and LifeSouth employees scrambled to look through its supply and provide as much as possible.
Thankfully, the hospital never needed all those units. The alert was sent as a precaution before the trauma center knew the exact amount of blood required.
In rare cases, UF Health searches beyond LifeSouth for a special type of blood for patients with super rare antigen types.
Pelletier said UF Health performed one national search and found only three units of blood that would work. One of those units failed the crossmatch, leaving only two units within the entire county that would work for the patient.
Each month, Pelletier said UF Health uses 300 units of cryo, more than 700 units of platelets and at least 2,200 red blood cell units.
UF Health rechecks the blood type once it receives units. Then the units wait in freezers until a department makes an order.
If the order is for red blood cells, a crossmatch check is done. Then the unit is placed in a fridge before being transported and used.
The blood ends up a long way from the original donor, but the units return to their original use, keeping the body running.
Suggested Articles
No related articles found.



