
In Zona Gale’s world, taking care of mom is a family affair—one that involves four generations of women in her household, including 90-year-old care receiver Joan Tompkins, Gale’s mother.
Tompkins had been living independently in a facility in Ft. Myers. But after a series of falls in 2020, Gale decided it was time for her mom to come home and be with family. She talked it over with her daughter and granddaughter in Gainesville, and everyone was of the same mind.
So, on Mother’s Day 2021, Tompkins reunited with her family for full-time caregiving, in a room of her own in her daughter’s home.
“Her two granddaughters packed me up and brought me home,” Tompkins said. And Tompkins said she is happy and well-cared for there by her family.
“Of course, I get all the attention,” she said with a smile.

The Administration for Community Living, part of the U.S. Department of Health and Human Services reported that in 2019 at least 53 million people were providing informal, usually unpaid, care and support to aging family members and people of all ages with disabilities (including mental health conditions) in 2019.
Assistant U.S. Secretary for Aging Allison Barkoff said in her introduction to the 2022 report by the National Strategy to Support Family Caregivers that steps are being taken “to ensure that family caregivers—who provide the overwhelming majority of long-term care in the United States—have the resources they need to maintain their own health, well-being and financial security while providing crucial support for others.”
“Lost income due to family caregiving is estimated to be a staggering $522 billion each year,” she wrote. “When family caregivers no longer can provide support, the people they care for often are left with no choices except moving to nursing homes and other institutions.”
Tompkins is staying this month at her granddaughter’s home along with Gale and one of Tompkins’ great-granddaughters, Arielle Barnard. Gale is still working as an academic technician specialist at Santa Fe College while helping care for her mom, but she may soon need some surgery of her own.
“I don’t want mom to go into a health care facility,” she said. “When I get stressed out or like this with problem with my knee, they step in and whisk her away.”
Tompkins was able to get around with a walker when she first arrived, but she is now limited to a wheelchair. Twenty-three-year-old Barnard is happy to do her bit to help.
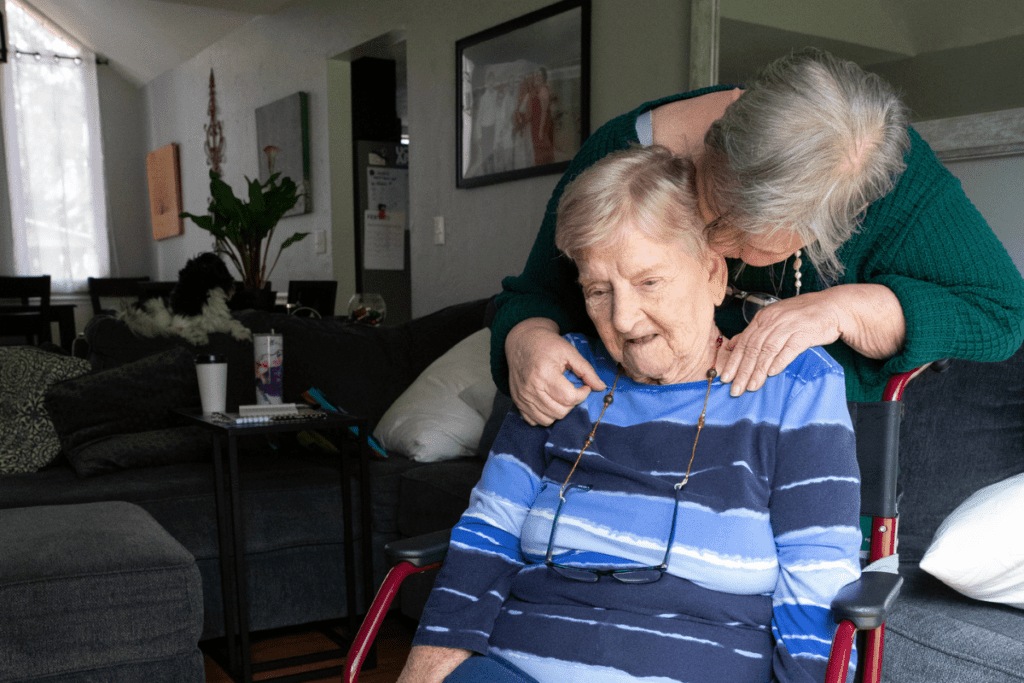
“I like it,” she said. “I like being there for her. Sometimes it feels like it just goes back and forth. It’s like what she would have done for me, it feels like the natural course of life.”
Family caregivers make up approximately 18% to 22% of the U.S. labor force, and according to data from the Rosalynn Carter Institute for Caregivers, close to a third of caregivers have voluntarily left a job to provide that care.
After his father died and his mother became ill, 73-year-old Alan Dychtwald moved from New Jersey to stay with his mother, Pearl, in Delray Beach. He and his brother Ken Dychtwald, a well-known gerontologist, decided to divvy up caregiving responsibilities with Alan acting as the point man on the ground and Ken providing more financial support.
Alan had been coming to Florida for years and in 2013 was there on a routine visit, just before his dad, Seymour, died at the age of 92.
“Immediately, I just came to Florida to be a caregiver because I was not going to leave my mother alone,” he said. “Even though there was someone here from 9 to 5, that wasn’t enough. I did not want to ever leave her alone.”
The two brothers are very close and speak with each other daily.
“I was going to live in Florida,” Alan said. “My brother had more money than me. He was going to supply the money, and I was going to supply the labor.
Family caregiving has become more prevalent as the cost of institutional care is spiraling, while long term health insurance is something that most people don’t have. While financial assistance for caregivers is important, industry experts say personal support programs to help caregivers readjust their lives to deal with their new realities may be even more critical.
Dr. Reetu Grewal, associate professor of family medicine at UF Health Jacksonville, considers self-care essential.
“There is a stress that people experience when giving and caring for other people,” she said in an interview. “It starts simple when doing one or two things for somebody. But it can grow. And suddenly that person is drawing from an empty well, which is when burnout sets in.”
Grewal said caregiver guilt is real.
“There is a lot of that that goes on,” she said. “And then we see the burnout because of it. I’m not giving enough. I need to do more. But if you don’t take care of yourself, how are you going to take care of someone else?”
Teri Lonon gives caregiving classes at Elder Options, and one of the things she emphasizes most is self-care for caregivers.
“It’s essential for them to take care of themselves,” she said. “You can’t pour out of an empty cup.”
Lonon said she finds that married caregivers sometimes have the hardest time adjusting to their new roles.
“What’s most stressful is their role and their relationship with the person has completely changed. When your relationship started with this person, you had certain expectations,” she said. “When you become caregiver of the person you have a relationship with, the relationship dynamics are completely changed, and your expectations are changed. That’s what causes the most stress because it is such an adjustment.”
Carolyn Alcantara, 63, said she found this to be true after her husband was diagnosed with mild Alzheimer’s disease. She signed up for the course at Elder Options and said it kept her from feeling so alone knowing she was part of a community of people who “got this [caregiving] dropped in their lap, too.”
Alcantara said when her husband first became ill, she was very angry “because he changed. I felt him to be kind of weak because he couldn’t remember stuff. That was me as a spouse and I had to get out of my vocabulary, words like ‘don’t you remember.’ These classes helped me learn coping skills.”
Sometimes home health care agencies can assist family caregivers by providing skilled nursing assistance or simply personal care.
Christina Ramos, executive director of Touching Hearts at Home, says her agency was founded by her family after her grandmother was diagnosed with Alzheimer’s more than a decade ago.
“We provide personal care services, activities of daily living, light housekeeping transportation, and engagement,” Ramos said. “Engagement is so important. Sometimes [when engaging with someone with dementia] people either talk too loud or too slow, so not everything is clear.”
Ramos said communication and engagement strategies are important: “We want our caregivers to be engaged.”
But there is still much more to do to assist family caregivers to adjust to new realities, including how to handle the many challenges of dealing with health care issues outside of home.
In a talk to fellows of the Columbia University Age Boom Academy, Jennifer Olsen, CEO of the Rosalynn Carter Institute for Caregivers, pointed out that it is critical not to think of caregiver issues in a box by themselves.
“The diagnosis of a person defines the support a caregiver gets,” she said. “Many caregivers are blocked from receiving services and support because they don’t have the right diagnosis. Doors get closed effectively.”
She said caregivers need to become knowledgeable about health literacy and payment literacy as well as insurance literacy and finance.
“When do I get what I need?” she said. “That in and of itself would unlock so many other stressors.”
Editor’s note: This is the fourth story in Mainstreet’s Aging Matters series. It was independently reported by Ronnie Lovler and underwritten by Elder Options. Some reporting was made possible by Lovler’s acceptance as a fellow into the 2022 Age Boom Academy, a program of the Columbia Journalism School, the Robert N. Butler Columbia Aging Center, and the Columbia Mailman School of Public Health.
Suggested Articles
No related articles found.




A good adult day care program can both help family caregivers avoid burnout and provide quality care, social experiences and mental and physical stimulation.
One excellent program is Altrusa House in Gainesville, which serves adults 18 and over who have physical or cognitive disabilities that require 24/7 care.
Check it out at Altrusa House.com, where you can visit it via a video or in person.