Our story is no different than thousands of other families who tangled with COVID-19 and were lucky enough to come out on the other side of it alive—without spending time in an ICU.
But the virus took us on a journey that we were not ready for.
We are an active couple. I am 54 and carry camera gear as I run up and down football fields with ease. My husband Aaron, age 49, is a former offensive lineman, track star and high school wrestling champ, who now works as a loader at a hardware store. He walks many miles every day, loads appliances into vehicles and helps contractors load pickups with bag after bag of cement mix.
On our off days, we like to run around Disney or Universal Orlando as pass holders, or take the kayaks out on the Santa Fe River, or head to a beach and take long walks.
But for the past five weeks we have been holed up in our house wondering when life will get back to normal.
I have been reporting on the COVID-19 pandemic since March. I have interviewed nurses from Gainesville on the frontline in New York City. I have interviewed renowned epidemiologists from UF Health and have been following COVID-19 survivor groups and long hauler research very closely.
And because of that, I knew that when my husband’s fever, chills and cough started on Dec. 10th, that COVID-19 had found us.
Our first move in the strategy to beat the virus started months ago when we upped our vitamin and supplement regimen. We both had been taking our temperatures every morning, that’s why we were able to spot the spike right away. We were taking vitamins C, D, B-6, B-12, K2, plus Zinc and Benadryl daily.
Once my husband displayed symptoms, he called in sick from work and I stocked up on electrolytes, soups, ginger ale, and purchased an oximeter to measure blood oxygen levels and heart beats per minute.
Aaron scheduled a telemedicine appointment with UF Health to line up a COVID-19 test and we masked up and divided the house into his and hers areas. He got the back bedroom and bath, I got the front.
Early on, Aaron lost his sense of taste, his fever was climbing and fatigue set in along with coughing. His test came back positive on Dec. 15, just as the vaccine for this virus was arriving in Gainesville.
We found the timing ironic and made sure to let employers and the short list of people we spent time with recently know that he had tested positive for COVID-19 so that they could monitor for symptoms. My visits to my 80-year-old mother stopped. I did not open up our thrift shop in Newberry. We did not leave the house after I took a test and it came back negative on Dec. 17th.
Now it was a wait-and-see game. How vicious of a wrath would this virus inflict on Aaron, and how long it would take for me to get it too?
I assumed that even wearing face masks would not keep me from getting the virus because we were sharing living space. I was checking Aaron for fever and bringing him meals, and the virus is so contagious. All I could hope for was that I was exposed briefly and in small doses and that would translate to a less severe case than what my husband had.
On Dec. 20, I knew it was my turn when I couldn’t taste my orange juice. For me, the symptoms were burning eyes and tongue, no taste, a runny nose and headache, fatigue, fever, and gastric issues that included nausea and bloating. It had very little impact on my lungs, although I had an intermittent dry cough.
At this point, my sister had come up from South Florida to help with our mother. She was bringing groceries and hot meals so that I didn’t need to leave the house at all.
As Aaron’s symptoms continued to worsen, I was up every two hours feeling his forehead as he slept. I listened to his breathing, which was becoming more labored.
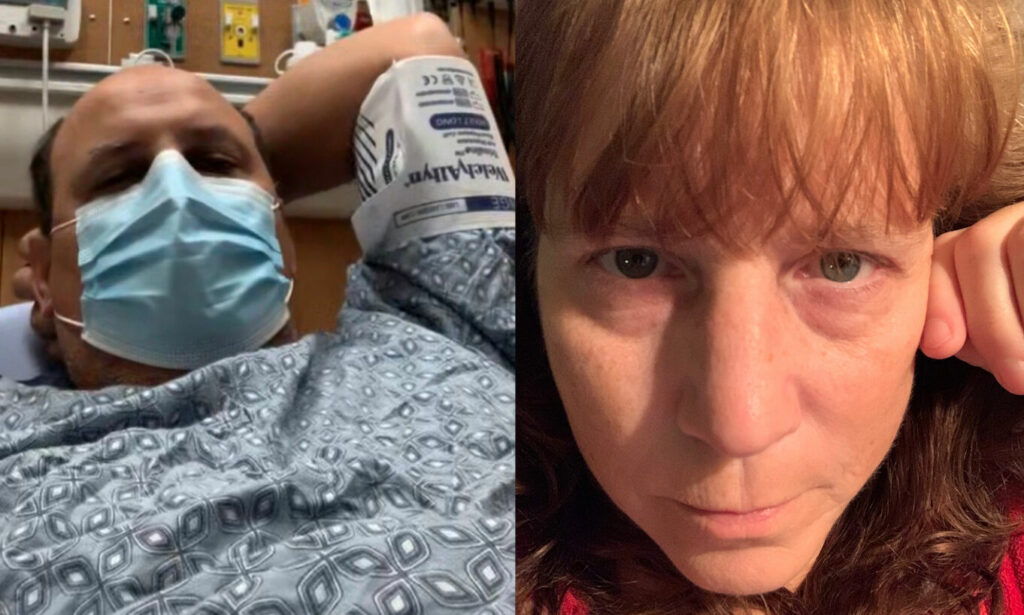
Five days after testing positive, Aaron was really having trouble breathing. His fever was 101 and rising, his blood oxygen level was on the decline. His heart rate was all over the place from 70 BPM to 110 at times. It was time to get help, so we headed to UF Shands Springhill Emergency.
Of course I was not allowed in the building as Aaron notified the admission clerk that he was COVID-19 positive and having trouble breathing. This was the scariest part of the journey—not knowing what would happen next.
I remember thinking: What if I see him wheeled out and that is the last time I set eyes on my husband?
I couldn’t just sit in my car and wait. It was a very real possibility that if doctors couldn’t get his vitals on track that he would be taken away in an ambulance to the main hospital.
So I sat on a cement table overlooking the ambulance bay and FaceTimed with my husband in between his chest X-ray and EkG.
During that time I saw people wheeled out and whisked away via ambulance. I remember thinking: What if I see him wheeled out and that is the last time I set eyes on my husband?
I had to go there and then bring myself back out of that possibility. Those saying COVID-19 is just the flu need to stop. I knew the virus could surge violently after the first week and was afraid that he might not be able to fend it off.
We got lucky. After doctors administered steroids, Aaron’s breathing was much better. They ran tests on his heart looking for signs of a potential heart attack and chemicals released by the body when the heart is under duress.
We returned home and continued with rest and opening doors and windows during the day to keep fresh air circulating, and changing sheets and pillow cases frequently. We stayed hydrated and rested as much as possible.
The good news—Aaron tested again and was negative on Jan. 4th. A few days later, on Jan. 9th, I also tested negative.
I added probiotics to my treatment and improved very quickly, and two weeks after the start of my symptoms am almost back to normal. No more fevers, taste returned, energy levels are back up.
But Aaron’s battle is far from over. A walk to the mailbox or even the refrigerator leaves him breathless. The fatigue and weakness continues. He returns to work soon and his doctor has modified his schedule to half days.
Studies have documented that COVID-19 can damage the heart, blood vessels, kidneys, brain, skin, eyes, and gastrointestinal organs. Many patients refer to having a brain fog afterward that affects their thought process and memory. We are both experiencing episodes of forgetting family members’ names and have trouble coming up with certain words when we are communicating.
Throughout this journey we relied heavily on the advice given by COVID-19 survivors on the two Facebook groups Survivor Corps and COVID-19 Long-Haulers Discussion Group. These forums are a collective of symptoms and recovery advice and also offer discussion groups and webinars about recovering from COVID-19.
The CDC also offers advice to those caring for someone that is COVID-19 positive.
I have canceled our future Thursday reservations to Disney parks and will need to find ways to spend our days off that involve less running around until Aaron makes progress in his recovery.
Our advice for anyone facing COVID-19 is to make sure you have a network of family and friends that can help out, stay up to date on treatments, monitor your symptoms and keep a journal. Watch for a possible surge during the second week, and seek care through your primary physician. Learn more about mitigating COVID-19 at CDC website.
If you have not come down with the virus, now is a good time to get a wellness check and have a full panel of blood work done and to adjust your diet and exercise plan so that your body is the best shape it can be in.
And don’t forget to register for the COVID-19 vaccine. Health care workers and people 65 and older are being offered inoculations. Visit the Alachua County Health Department website Florida Department of Health in Alachua for more information or contact your primary physician.

Suggested Articles
No related articles found.



